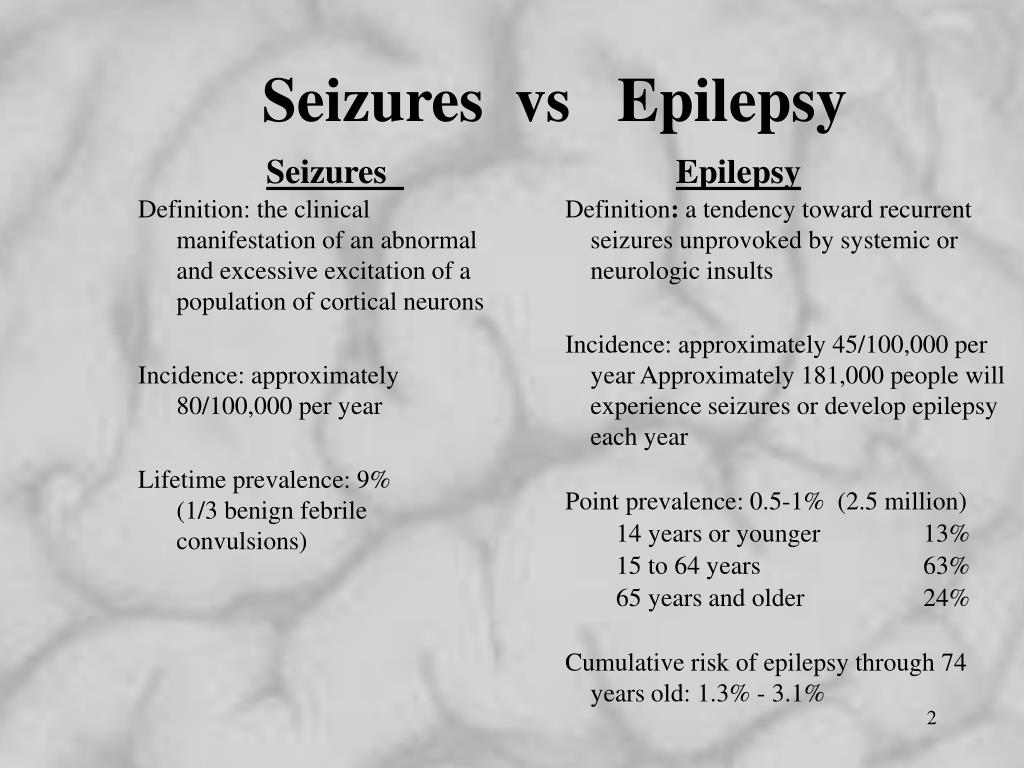
These precipitating factors tilt the balance between excitatory and inhibitory neurotransmissions which has been established in different types of epilepsy. These were due to known underlying factors that cause seizures such as brain damage ( Sizemore et al., 2018), metabolic diseases ( Tumiene et al., 2018), infections ( Bartolini et al., 2018), hemorrhagic stroke ( Zhao et al., 2018), and gene mutations ( Leonardi et al., 2018). The active annual prevalence, prevalence during lifetime and the incidence of epilepsy were found to be higher in the developing countries ( Fiest et al., 2017).Ī systematic review revealed that epilepsies of unknown etiology had the highest prevalence compared to the epilepsies of known origin ( Fiest et al., 2017). Meanwhile, the annual cumulative incidence of epilepsy was 67.77/100,000 persons and the incidence rate was 61.44/100,000 person-years. In early 2017, the point prevalence of active epilepsy was found to be 6.38/1,000 individuals, while the lifetime prevalence was 7.60/1,000 persons. Genesis of epilepsy is attributed to various predispositions that include neurological, perceptive, psychological, and social factors, which could either stimulate or worsen the syndrome. The International League Against Epilepsy (ILAE) published a recent clinical definition of epilepsy in which a patient with any of the following conditions is considered to be an epileptic i.e., (i) two or more unprovoked seizures within more than 24 h apart (ii) one unprovoked seizure and a probability of further seizures similar to the general recurrence risk, occurring over the next 10 years (iii) definite diagnosis of an epilepsy syndrome ( Fisher et al., 2014). An epileptic seizure is considered as a transient episode of signs or symptoms, including transitory confusion, staring speech, irrepressible jerking movements, loss of consciousness, psychic symptoms such as fear and anxiety, due to the abnormal synchronous neuronal activity of the brain. In the present review, we aim to discuss the predominance of sleep-related epilepsy during NREM, established familial links to the pathogenesis of SHE, BECTS and PS, and highlight the present available pharmacotherapy options.Įpilepsy is characterized by frequent and unpredictable disruptions of brain functions resulting in “epileptic seizures.” Epilepsy has a great impact on the quality of life through increased incidence of injury and death, unemployment rates, lower monthly incomes, higher household costs and high absenteeism at work and schools ( Jennum et al., 2017 Trinka et al., 2018 Wibecan et al., 2018). 
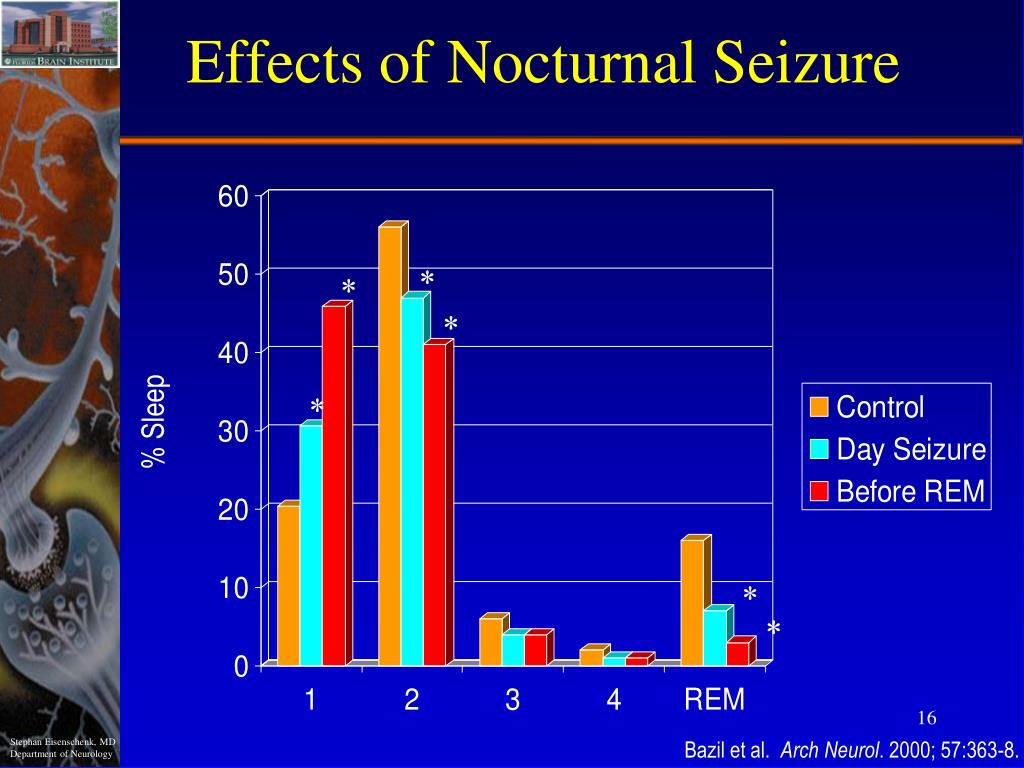
Although some familial types are described, others are seemingly sporadic occurrences. Sleep related hypermotor epilepsy (SHE), benign partial epilepsy with centrotemporal spikes or benign rolandic epilepsy (BECTS), and Panayiotopoulos Syndrome (PS) are three of the most frequently implicated epilepsies occurring during the sleep state. Current findings indicate that the sleep-related epilepsy manifests predominantly during the synchronized stages of sleep NREM over REM stage. Sleep comprises two distinct stages i.e., non-rapid eye movement (NREM) and rapid eye movement (REM) that alternate every 90 min with NREM preceding REM. Sleep-related epilepsy is nocturnal seizures that manifest solely during the sleep state. 
In the last several decades, sleep-related epilepsy has drawn considerable attention among epileptologists and neuroscientists in the interest of new paradigms of the disease etiology, pathogenesis and management.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
